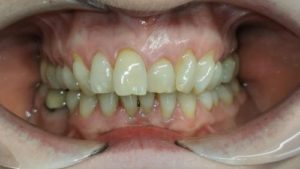
This patient had approached one of our dentists and requested to ‘straighten’ her teeth with Invisalign. At the outset of treatment, she was not concerned about the different height of the UL1 gingival margin. How do we manage such a request at the end of an initial course of treatment ? It is easy to fall into the trap of providing an ‘instant’ result, such as by crown lengthening which may not be in the patient’s best interest or may not manage her expectations.
Firstly, as this cosmetic dilemma was accepted at the outset, a new treatment plan needs to be devised to correct the deficiency, and this needs to be fully quoted for as extensive re-treatment will become necessary.
Let us examine the ‘key features’ of this case:
Treatment Option One – Crown Lengthening
Crown lengthening can be a quick fix for this case, but consider the risk. To equalise the gingival zeniths will require circa 3+ mm of osseous crest reduction at UL1 to accommodate the biologic width of periodontium and place this at the same level as UR1. The additional risk is unpredictable further recession as a result of surgery although the thick phenotype may mitigate this somewhat. The main aesthetic dilemma will be that the osseous reduction will result in loss of interdental papilla. We will open up the embrasures between the narrowing root of UL1 and there will be black triangles between UL1 and adjacent teeth. We would then need an extracoronal restoration placed on a root surface to develop the emergence profile and achieve a contact point no more than 5 mm coronal to the osseous crest to reliably close the embrasure (Tarnow et al, 1992). The next restorative dilemma is that if you are fabricating a ceramic restoration, you will need to keep the marginal preparation thin to avoid overly thinning the root surface. This could result in marginal fracture of lithium disilicate or even zirconia restorations that are fabricated to < 0.7 mm marginal thickness.
This option carries too many risks and dilemmas.
Treatment Option Two – Composite Build Up and Aligners
UL1 can be built to the correct physical dimensions in composite, the case rescanned, and Invisalign aligners used to attempt to intrude Ul1. This will put the gingival margin at the correct height to UR1. Unfortunately, an aligner can deflect across the the maxillary arch while attempting to intrude UL1 and this can have deleterious effects on archform. There are some case reports describing use of the Invisalign technique to intrude incisors, however most of these describe ‘relative intrusion’ techniques where the maxilary teeth are being retracted, or the mandibular incisors are being protracted. The case described above requires ‘absolute’ intrusion where no secondary effects as a result of dissipation of anchorage can be afforded on adjacent teeth.
Treatment Option Three – Aligners or a sectional fixed appliance with the assistance of TADS (Temporary anchorage devices)
The best approach to treatment is to push the UL1 into the alveolar bone gently using light continuous forces of up to 30 grammes. Anything more than this will risk hyalinisation and external apical root resorption (EARR). First a periapical radiograph of Ul1 is required to ensure good root form – there must not be a blunted root, a pipette shaped root, or a deviated root or a tapered root form – these root forms are prone to external apical root resorption (Malmgren and Levander). You need to satisfy yourself that there will be minimal EARR
![Deviating root forms [ after Levander and Malmgren (1988) ]. 1 , short... | Download Scientific Diagram](https://www.researchgate.net/profile/Irene-Aartman/publication/51483313/figure/fig1/AS:668481188028420@1536389743228/Deviating-root-forms-after-Levander-and-Malmgren-1988-1-short-root-2-blunt.png)
Secondly, UL1 should be built to ideal proportions in composite using a mono-chromatic build up technique.
Thirdly the case is scanned with instructions to Align that Ul1 is to be fully intruded. There needs to be a labial cut out to facilitate the placement of a button.
When you come to place the new set of aligners, bond a metal button as cervical on Ul1 as possible. This is to direct forces as close to the centre of resistance as possible and avoid significant protraction of UL1.
TADS can be placed on the mesial and distal buccal aspect of the alveolus adjacent to UL1. A button can be placed as cervically as possible. A light triangular conformation power chain is then placed from right TAD to button to left TAD to place a controlled intrusive force on UL1. The labial mechanics will result in some loss of anchorage and proclination of UL1 will occur, however this is desirable. The TAD mechanics could be supported by aligners to minimise proclination of UL1.
At the end of treatment, the composite on UL1 can be modified using a polychromatic technique to maximise aesthetics, and long term retention will be needed.
Reading Material